Beauty
Impetigo Risk Factors and Prevention

Do not let the water run on your hands. You should rub your hands together vigorously for at least 20 Impetigo is a highly contagious bacterial skin infection. It is common in children and infants, although adults can also become infected. The disease can cause sores all over the body that eventually burst and ooze, as well as fluid-filled blisters and honey-colored scabs on the body.
Some people with impetigo also develop deeper sores and blisters, which can be painful. This is known as etyma and can occur when impetigo is not treated.
Impetigo is not immediately dangerous or life-threatening if treated, but it can spread quickly among peers. It can become a problem in schools and sports teams.
As with other contagious skin diseases, it is possible to prevent impetigo and stop its spread. Prevention starts with understanding the cause of this skin infection and the risk groups.
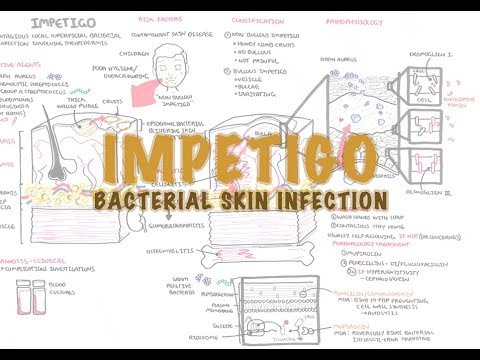
Most Common Causes Of Impetigo
Impetigo is a superficial infection usually caused by one of two bacteria: Staphylococcus aureus or Streptococcus pyogenes. Strep bacteria are the same bacteria that cause strep, while staph bacteria can be MRSA, a special strain that is resistant to many antibiotics.
If you have a skin injury, such as a cut or scratch, or if you have been bitten by an animal or insect, both bacteria can enter the skin and cause an infection in the top layer of the skin.
But this is not the only way to get impetigo. Because this condition is contagious, you can also become infected if you come into contact with the sores of an infected person, or if you share or touch objects that they have touched.
These elements may be:
- Sheets and covers
- Towels
- Loofah sponges
- Clothing
- Countertops and other surfaces
- door handles
Main Risk Factors For Impetigo that you should know
Although touching contaminated objects and surfaces can spread impetigo, some factors also increase the risk of this bacterial infection:
Age
Impetigo can affect people of all ages, including teenagers and adults. But it is more common in young children between 2 and 5 years old.
Proximity to another infection
Because skin-to-skin contact increases the likelihood of spreading impetigo to others, this condition can spread to places where people are in close contact with others. This also applies to schools and kindergartens. Impetigo can also spread from person to person at work and at home.
Hot and humid weather
The bacteria that cause impetigo thrive in moisture and heat. The risk of developing this skin condition increases in the summer, and cases of impetigo are more common in areas with hot and humid climates. In the United States, people tend to develop this disease in the summer or fall.
Participation in sports
As an athlete, you are no longer prone to impetigo. But if you play a sport that involves skin-to-skin contact with other players or the use of shared sports equipment, you are at a higher risk of getting this skin infection. Remember that you can only get impetigo if you have a skin injury or come into contact with someone who has the disease.
Damaged skin
Broken skin also provides an entry point for staph or strep bacteria. This includes washing the wounds, applying a topical antibiotic cream, and covering the wounds with an adhesive bandage or gauze and tape until they heal.
How to prevent the spread of impetigo?
Prevention of impetigo is not only aimed at preventing the infection from infecting other people, but also at preventing the infection from spreading to other parts of the body.
Impetigo is a skin infection that can go away on its own. “Even without medication, most cases of impetigo should clear up within two to three weeks,” says Rick Pescadores, DO, executive director of the Delaware Department of Public Health.
Treatment is recommended to avoid contamination of others. Antibiotics, especially topical ones, are often used for impetigo. Severe and widespread infections may require oral or injected antibiotics.
It takes some time for antibiotics to enter the body. So you remain contagious for about 24-48 hours after starting the medication.
Here are some tips to prevent impetigo from spreading to others and other parts of the body:
Do not share personal items. If a person with impetigo touches their sores and then touches an object, that object becomes infected. It is therefore important to avoid contact with contaminated surfaces. Do not share razors, towels, washcloths or other personal items. Remember that impetigo can also spread from person to person through toys. If you notice sores or blisters on someone that resemble impetigo, avoid physical contact with the person or objects they touched.
Disinfect surfaces. Disinfecting frequently touched surfaces is another way to prevent the spread of impetigo. If you work in a school or nursery, use disinfectant wipes on work surfaces, doorknobs, and light switches to reduce the risk of contaminating people. Take similar measures at home and keep frequently touched surfaces free of germs. Do not touch the sores or blisters. The less you touch your sores and blisters, the less likely the impetigo will spread to other parts of your body. Remember to wash your hands after treating your injuries. Use a disposable paper towel to dry your hands and do not reuse cloths.
Change the towel and hand towels every day. You can also stop the spread of the infection by using a clean towel and washcloth every time you wash. Wash sheets, sheets and towels in hot water.
Apply an anti-itch cream. Impetigo can be itchy and it is important not to scratch the lesions as bacteria can get under the nails and spread to other parts of the body. Apply an anti-itch remedy to the lesions (wash your hands afterwards) and clip your nails to avoid damaging the skin, which can make impetigo worse.
Keep wounds clean and covered. Accidental contact with someone with impetigo can also spread the infection. If your child has injuries, be sure to cover the sores or blisters with gauze and duct tape until the skin heals. Covering wounds can also protect other family members, especially when sharing a bed with an infected person.
Unfortunately, even after the impetigo has healed, it is possible for the infection to return. Following the tips above will also help prevent reinfection – don’t share personal items, treat wounds appropriately, and avoid skin-to-skin contact. You can also protect yourself by showering after each workout to remove bacteria from your skin.
When treating impetigo, make sure to wear only clean clothes and wash all worn clothes in warm water. Also wash your hands often with warm, soapy water, especially after shaking someone’s hand.
Be sure to practice proper hand washing techniques. seconds. The correct way to wash your hands is:
- Wet your hands with running warm water.
- Apply the soap and rub your hands together to create a lather.
- Rub your hands together for at least 20 seconds.
- Rub the front and back of your hands and between your fingers.
- Rinse your hands with clean water.
- Dry your hands with a clean towel.
Sometimes you don’t have access to water or soap. If not, protect yourself with an alcohol-based hand sanitizer. Make sure the product contains at least 60 percent alcohol.
Soap and water are best, but sanitizers can reduce bacteria on your hands and help reduce the risk of bacterial infections.
Apply the gel correctly, pour a small amount on the palm, rub your hands together and let your hands air dry. It takes about 20 seconds to apply the hand sanitizer from start to finish.
A final word on impetigo: skin infections can be prevented
Impetigo often looks worse than it actually is, but while this is not a particularly dangerous skin condition, there is a risk of complications if left untreated.
It can lead to permanent scarring on the skin and kidney infections. Impetigo can also lead to cellulitis, an infection that affects the subcutaneous tissue. This infection can also spread to the lymph nodes and the bloodstream and be life-threatening.