Health
Does Medicare cover dementia care?

Does Medicare cover dementia care?
Both Original Medicare and Medicare Advantage cover dementia costs, but the prepayment and coinsurance waivers differ between the two programs.
Physical changes in the brain cause depression, a progressive condition. As the symptoms worsen, the patient needs different treatments and care.
Medicare helps pay for certain services at all stages of dementia. Insurance areas include tests that assess a person’s thinking ability, home medical care, prescription drugs and hospital treatment.
This article describes dementia and examines Medicare coverage from early to advanced stages of the disease. This article also lists dementia-related services that are not covered by Medicare.
Does Original Medicare cover dementia care?
Medicare supports the services that people with dementia need at all stages of the disease. The chart below provides an overview of Medicare coverage for people with dementia. More information on the lighting of each section is provided below.
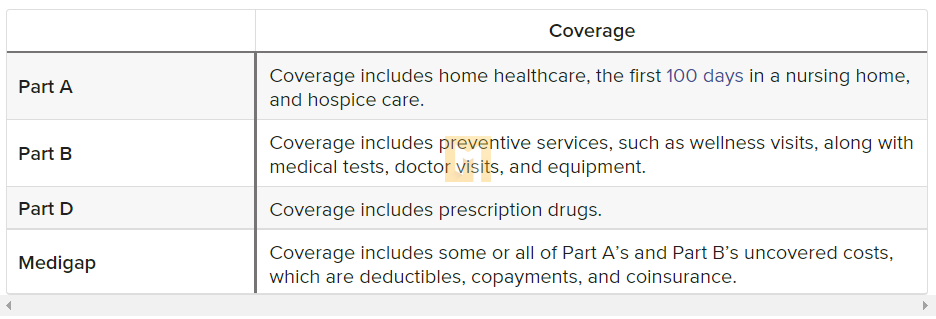

Does Medicare cover dementia care?
Original Medicare (Part A and Part B)
Original Medicare offers insurance coverage for different stages of dementia.
Health tips
Medicare coverage for dementia can begin before the disease develops. When doctors visit the health center every year, they may notice the first signs of dementia.
The health process includes creating a personal plan to prevent illness. Doctors make plans based on the individual’s health status and risk factors, taking into account the following points:
- Family and personal history
- Prescription drugs
- Measure height, weight and blood pressure
- Signs or symptoms of dementia
If the dementia is of some degree, the individual plan may include treatment options. He or she may also recommend lifestyle measures such as:
- Eat nutritious food
- Exercise regularly
- Participation in social activities
- Participate in emotional activities such as crossword puzzles
Early Dementia
In the early stages of dementia, many people benefit from living in their own home.
Medicare Part A pays for up to 35 hours per week of home care for people certified as home care providers.
Part B covers testing, doctor visits and medical supplies.
There is no waiver or coinsurance, but a 20% coinsurance covers doctor visits, supplies, and other medical tests. In addition, the Section B exemption of $203 per year applies.
Later Dementia
In the later stages of dementia, people are often unable to stay at home. At this stage, they usually need 24-hour care.
Part A covers the first 100 days in a skilled nursing facility (SNF). A SNF is a provider of nursing or nursing care services. This care differs from care in a nursing home, where a person can be helped to wash, dress or eat, but no medical or nursing services can be provided.
This price does not include licensing. 1-20 days are not covered by penny insurance. From the 21st to the 100th day, the price is $185.50. After 100 days, that person is responsible for all expenses.
Medigap is a supplement to Medicare. A Medigap plan helps cover the unknown costs of Medicare Parts A and B, including coinsurance such as deductibles, prepayments, and professional care.
Fear of the end of life
If a doctor determines that a person with dementia has 6 months or less to live, Medicare will pay for palliative care.
This coverage includes medical, nursing and personal care services, as well as consultations and prescription drugs. Coverage is not location-based and does not depend on whether a person receives care at home, in a nursing home, or in a nursing home.
This cost does not include a deductible and coinsurance is minimal.
Do Medicare benefits cover dementia?
Medicare Advantage (Part C) plans replace Original Medicare.
Part C provides dementia services covered by Medicare Parts A and B. Plans may also include additional benefits such as travel to doctor’s appointments. However, deductibles, deductibles and co-insurance may differ from basic insurance.
One type of benefit plan, a special needs plan, offers specific benefits for chronic conditions, including dementia.
While Primary Medicare coverage is fixed, Medicare Advantage plans can vary greatly. A person should carefully read the explanations of the benefits of each policy when deciding which option is best for them.
What dementia services are not covered by Medicare?
While Medicare helps cover the health care costs associated with dementia, it does not cover everything a person may need. Services not covered are:
- 24-hour home help
- Care at a qualified care facility after the first 100 days
- Kindergarten for adults
- Incontinence care
- Food delivery service
- Personal hygiene, such as bathing and dressing, if this is the only care the person needs
- Housekeeping, such as washing and shopping, if the person simply needs care
- Food supplements
Summary
Health insurance for a person with dementia starts with preventive treatment in the form of an annual health check-up.
If a person has dementia, insurance can help cover costs as the disease progresses. This insurance includes palliative care in the last months of life.
Whether people had an Original Medicare plan or a Medicare Advantage plan, they are entitled to coverage. But the two programs have different deductibles, copayments, and coinsurance costs. Those who are unsure of the details of their coverage should talk to their plan provider.